Pain has a way of negotiating with you. It starts small, showing up after a long walk or a night of poor sleep, and you talk yourself into waiting it out. Maybe it’s just a flare-up. Maybe it’ll pass. But hip pain, left unaddressed, doesn’t negotiate in your favor forever. It compounds.
The joint you’re protecting by avoiding the doctor’s office is the same one quietly deteriorating while you wait. And what begins as occasional discomfort can become something far more complex to unwind.
The Biology of a Joint That’s Been Waiting Too Long
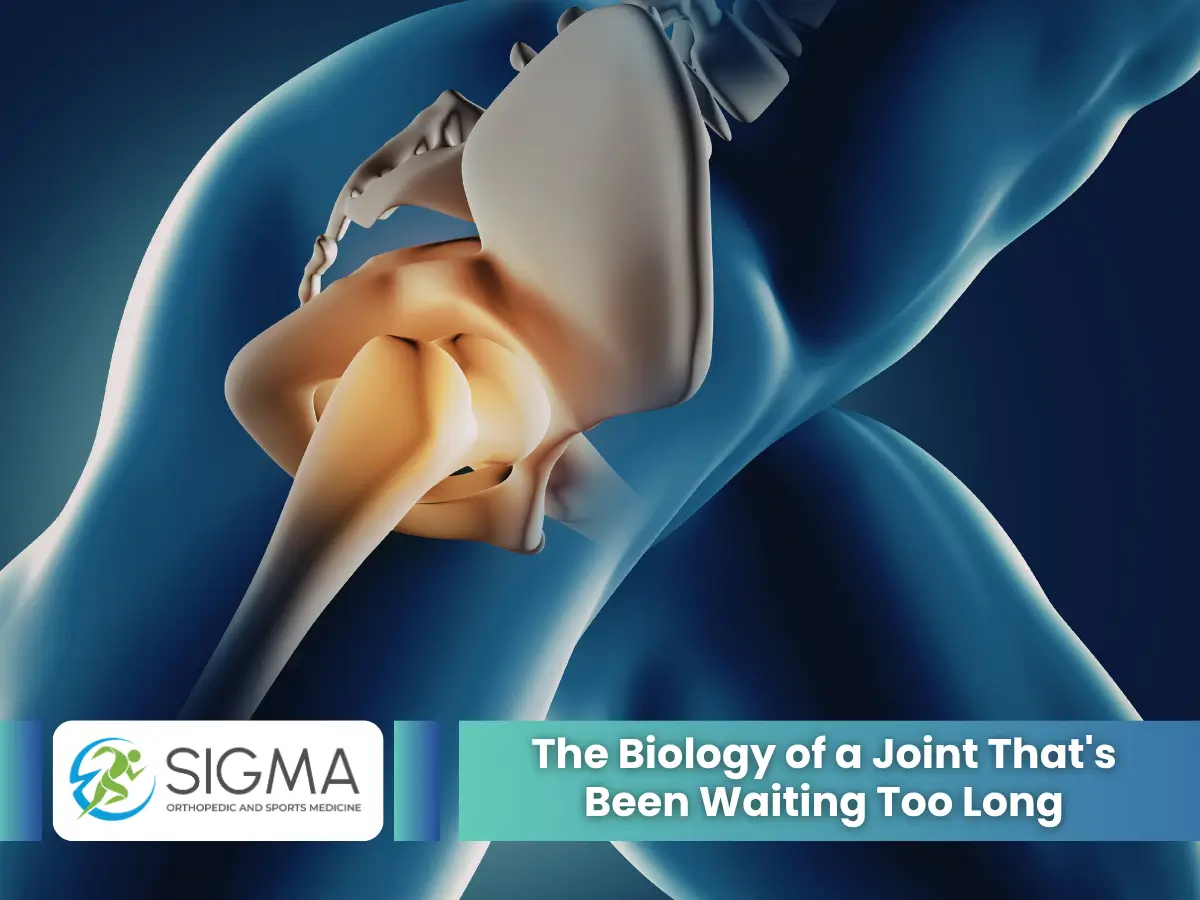
The hip joint is a ball-and-socket structure. It carries roughly three times your body weight with each step and five to six times with a stair climb, according to data from the American Academy of Orthopaedic Surgeons. That’s a lot of mechanical demand on a joint that relies on cartilage, labrum, synovial fluid, and surrounding musculature all working in sync.
When pain enters the picture, and you don’t pursue treatment for hip pain, your body compensates. You shift your gait. You favor one side. You avoid certain movements. This compensation cascade doesn’t protect the hip. It just redistributes the stress, loading the knee, the lumbar spine, and the opposite hip in ways they weren’t designed to absorb long-term.
Research published by the National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS) confirms that joint damage from untreated conditions like osteoarthritis is largely irreversible. Cartilage doesn’t regenerate the way muscle does. Once it’s gone, it’s gone.
Hip Flexor Pain Treatment: Why That Nagging Tightness Deserves More Respect
A lot of people misread hip flexor pain as a minor muscular issue and reach for a foam roller. Sometimes that’s appropriate. But chronic hip flexor pain treatment needs a more layered approach, especially when the tightness is accompanied by groin discomfort, clicking sensations, or pain that radiates down the thigh.
The psoas and iliacus, the primary hip flexors, connect the lumbar spine to the femur. When they’re chronically tight or inflamed, they don’t just hurt in isolation. They pull on the spine, affect pelvic tilt, and create a chain reaction of compensatory patterns. Treating that pain as purely muscular, without a proper diagnostic workup, is where a lot of patients lose time.
What looks like a tight hip flexor might be a labral tear, femoroacetabular impingement (FAI), or early-stage arthritis. Each of those conditions has a different treatment trajectory. The longer you wait to find out which one it actually is, the fewer non-invasive options remain on the table.
Perimenopause Hip Pain Treatment: The Hormonal Factor Most Clinics Miss
Women navigating perimenopause often notice joint changes they weren’t warned about. Hip pain, stiffness upon waking, and a new ache that didn’t exist two years ago. It’s not imagined. Estrogen plays a direct role in maintaining cartilage integrity and joint lubrication, and as levels fluctuate during perimenopause, joints can become more vulnerable to inflammation and wear.
The Office on Women’s Health acknowledges musculoskeletal changes as an underreported symptom of menopause. Yet most women who show up at a general practitioner with hip pain during this transition get told to rest, take ibuprofen, or come back if it gets worse.
That’s not perimenopause hip pain treatment. That’s deferral. A proper evaluation should factor in the hormonal context alongside imaging and functional assessment. The approach to care during this window is different from what a 30-year-old athlete or a 70-year-old retiree needs, and it should be treated as such.
Front Hip Pain Treatment: The Location Tells a Story

Not all hip pain points to the same source. Where you feel it matters. Front hip pain, that ache or pinch you notice when you sit down, climb stairs, or lift your knee, typically signals something different from lateral or posterior hip pain.
Anterior hip discomfort is often associated with:
• Labral tears, particularly in active adults who rotate and flex repeatedly
• Hip flexor tendinopathy or bursitis
• Femoroacetabular impingement (FAI), where bone spurs create friction during movement
• Early-stage hip osteoarthritis, especially in women over 45
Front hip pain treatment that skips imaging and jumps straight to physical therapy can occasionally help, but it can also reinforce compensatory movement patterns that worsen the underlying issue. An accurate diagnosis isn’t bureaucratic caution. It’s the difference between eight weeks of PT that solves the problem and eight months of PT that doesn’t.
Hip Pain Treatment Without Surgery: What’s Actually Possible
The assumption that serious hip pain inevitably leads to surgery stops a lot of people from seeking care early. That assumption is outdated. Hip pain treatment without surgery is a well-established, clinically supported pathway for many conditions, especially when caught before structural damage becomes severe.
Evidence-based non-surgical options include:
• Targeted physical therapy with a structured protocol, not generic strengthening
• Corticosteroid or hyaluronic acid injections for inflammatory joint pain
• Orthobiologic therapies such as platelet-rich plasma (PRP), which show promising outcomes in early to moderate cartilage degradation
• Activity modification and gait retraining
• Anti-inflammatory nutritional strategies and weight optimization
According to NIH’s National Library of Medicine, PRP and other orthobiologic treatments have demonstrated statistically significant improvements in pain and function for hip osteoarthritis patients compared to placebo controls.
The window for non-surgical intervention doesn’t stay open indefinitely. Joint damage that’s addressed at stage two doesn’t require the same level of intervention as damage that’s been allowed to progress to stage four. That’s not a scare tactic. It’s mechanics.
Treatment for Hip Joint Pain: What a Proper Evaluation Actually Looks Like
Most people have experienced a medical encounter where they talked for eight minutes, got a referral slip, and left more confused than when they arrived. That kind of surface-level interaction isn’t treatment for hip joint pain. It’s triage.
A proper evaluation for chronic or complex hip pain should include a thorough movement assessment to identify the actual pain generator, not just the area of complaint. It should include an imaging review by someone who understands the relationship between radiographic findings and clinical symptoms. And it should produce a clear answer: here’s what’s happening, here’s why, and here’s the path forward.
That kind of clarity isn’t common. It requires time, clinical precision, and a team that communicates across specialties. When those elements are present, patients don’t just get a diagnosis. They get a roadmap.
Why SIGMA Orthopedics Approaches Hip Pain Differently

At SIGMA Orthopedics, hip pain isn’t treated as a standalone complaint. It’s evaluated within the full context of a patient’s movement patterns, medical history, imaging, and life demands.
The SIGMA approach draws on Six Sigma methodology, a precision framework originally developed in manufacturing and aviation to minimize error and maximize predictability. Applied to orthopedic care, it means every patient moves through a structured pathway: precision diagnosis, personalized treatment options, and measured outcomes tracked at every milestone.
Where most clinics operate by intuition and convention, SIGMA operates by protocol. That distinction matters when you’re dealing with a condition as mechanically complex as hip pathology.
The SynerG Orthobiologics program, developed in-house, integrates evidence-based regenerative treatments directly into care pathways for patients who are candidates for non-surgical intervention. It’s not an add-on. It’s woven into the clinical decision-making process from the start.
And because hip pain rarely exists in isolation, the team at SIGMA, spanning sports medicine, spine specialists, and rehabilitation, collaborates across disciplines. You don’t have to coordinate your own care between three separate offices. That coordination happens within one system.
Conclusion:
Every week of delayed hip pain treatment is a week of compensatory movement, progressive joint stress, and narrowing treatment options. That’s not pessimism. It’s physics.
The good news is that most hip conditions, caught in time and evaluated properly, have real, non-surgical pathways to resolution. But that window requires action. Not urgency for its own sake. Just the recognition that your joints aren’t waiting for you to feel ready.
If you’ve been managing hip pain on your own and it isn’t resolving, a structured clinical evaluation isn’t a last resort. It’s the logical next step.
Ready for answers, not guesses? Book a consultation at SIGMA Orthopedics and get a structured evaluation designed to identify the actual source of your pain. Call 833-SIGMA-MD or request an appointment online.
Frequently Asked Questions
How long is too long to wait before seeking hip pain treatment?
If hip pain lasts more than 4–6 weeks without improvement or starts affecting walking, sleep, or daily activities, it shouldn’t be ignored. Persistent pain or changes in movement patterns signal the need for a clinical evaluation.
Can hip flexor pain treatment be done at home, or does it always require a clinic?
Mild hip flexor pain from overuse or sitting can improve with stretching, strengthening, and rest. However, sharp or persistent pain with symptoms like clicking or locking needs professional evaluation to rule out deeper issues.
Is there an effective treatment for hip joint pain during perimenopause without surgery?
Yes, many non-surgical options like physical therapy, anti-inflammatory care, injections, and PRP can reduce pain and improve mobility. The right treatment depends on understanding hormonal and structural changes together.
What makes front hip pain different from other types of hip pain?
Front hip pain often points to issues in the joint itself, such as labral tears or hip impingement. Unlike side or back pain, its location helps guide accurate diagnosis and targeted treatment.
What should I expect at my first hip pain consultation at SIGMA?
Your visit includes a detailed movement assessment, medical history review, and imaging analysis if needed. You’ll receive a clear diagnosis and a structured treatment plan with defined next steps.




