Surgery is surgery, right? You go under, something gets fixed, you wake up, and eventually walk out. That’s the version most people carry into their first orthopedic consultation. But when it comes to the hip, that framing misses something important. The distance between hip arthroscopy and traditional open surgery isn’t measured in incision length alone. It’s measured in recovery time, complication rates, joint preservation, and frankly, the entire philosophy behind how the problem gets approached.
This isn’t about one being categorically better than the other. Both have their place. What matters is understanding which one fits the actual condition and why that distinction changes everything that follows.
Two Approaches, Two Different Surgical Worlds
Open hip surgery involves a significant incision, retraction of surrounding tissue, and direct visualization of the joint. It’s the traditional method and still the appropriate choice for conditions like severe arthritis that have progressed beyond the reach of minimally invasive techniques.
Hip arthroscopy works differently. A surgeon inserts a narrow camera and specialized instruments through small portals, typically two or three, and operates while viewing a high-definition image on a monitor. The joint is accessed without the level of soft tissue disruption that open procedures require.
The practical difference shows up almost immediately after surgery. Patients who undergo arthroscopic procedures generally experience less postoperative pain, reduced blood loss, lower infection risk, and a faster return to normal activity. That’s not a marketing claim. It reflects the mechanical reality of how much tissue is disturbed to reach the problem.
Hip Arthroscopy Labral Repair: Precision Where It Counts
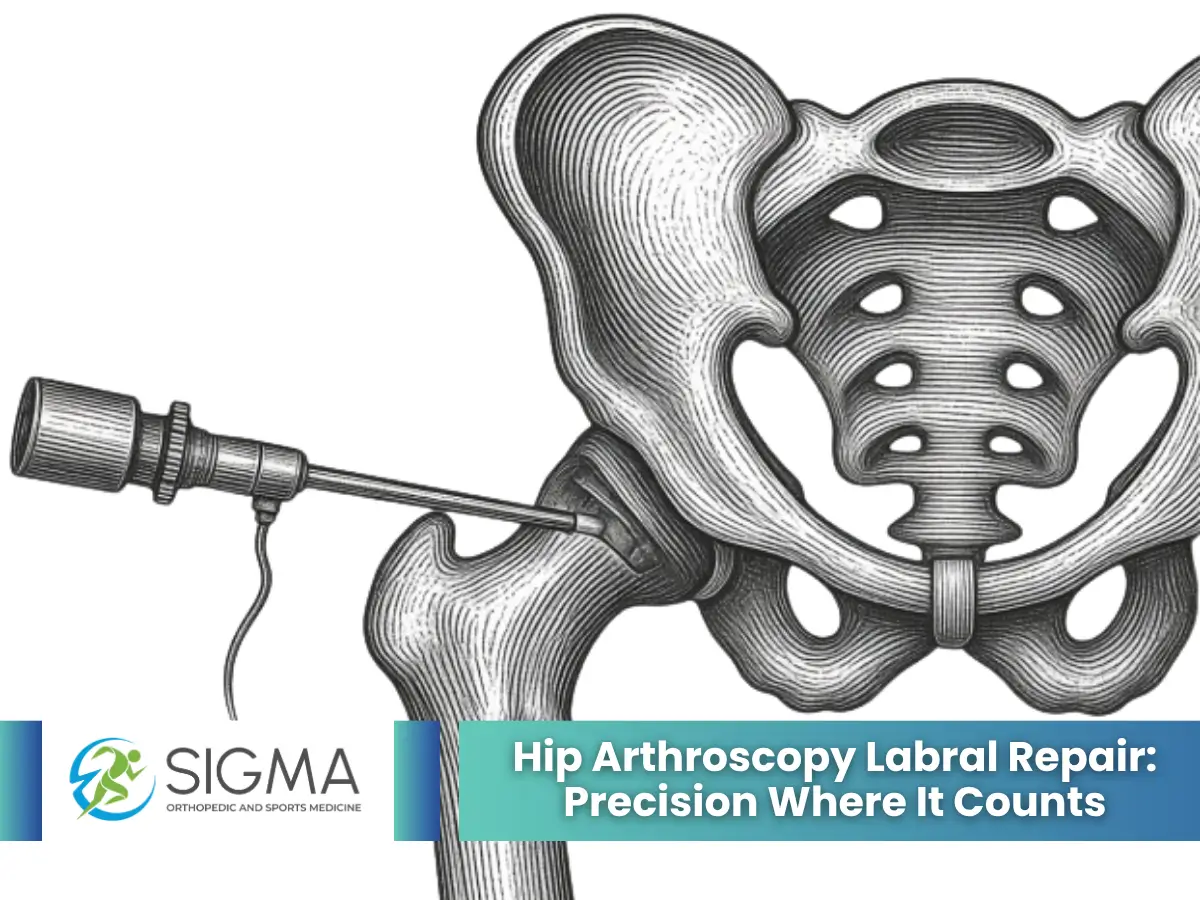
One of the most common reasons patients end up having an arthroscopic procedure is a torn labrum. The labrum is a ring of cartilage that lines the hip socket, sealing the joint and distributing load across the articular surface. When it tears, typically from repetitive hip flexion, a structural impingement, or a direct injury, the joint loses both stability and cushioning.
Open surgery to address a labral tear involves considerable exposure and carries a higher risk of disrupting the surrounding structures that keep the hip functioning normally. Arthroscopic labral repair, by contrast, allows a surgeon to access, reattach, and reconstruct the labrum with minimal collateral disturbance. Research published by the American Journal of Sports Medicine has consistently documented favorable outcomes for arthroscopic labral repair, particularly in younger and physically active patients, where joint preservation is the clinical priority.
What arthroscopy makes possible here isn’t just a smaller scar. It’s a fundamentally different ability to protect the surrounding tissue while addressing the actual source of pain.
Hip Arthroscopy Recovery Time: Setting Honest Expectations
Recovery from hip arthroscopy is measured in phases, not a single timeline. And this is where a lot of patients get frustrated, not because the recovery is harder than expected, but because nobody gave them a map before they started.
A general framework for arthroscopic hip recovery looks something like this:
• Weeks 1 to 2: Protected weight-bearing with crutches, managing swelling, beginning passive range-of-motion work
• Weeks 3 to 6: Progressive weight transfer, introducing active movement, initiating formal physical therapy
• Weeks 6 to 12: Strengthening phase, gait normalization, building functional endurance
• Months 3 to 6: Sport-specific or activity-specific conditioning, depending on the patient’s goals
Compare that to recovery from open hip procedures. A total hip replacement, even with modern surgical techniques, typically involves a longer protected period, more significant restrictions on movement, and a rehabilitation process that extends considerably further. The starting point is simply further from the function.
Hip arthroscopy recovery time isn’t short by any standard. But the trajectory is steeper, and the ceiling is higher, particularly for patients who were active before their injury.
Hip Arthroscopy vs. Total Hip Replacement: Not the Same Conversation
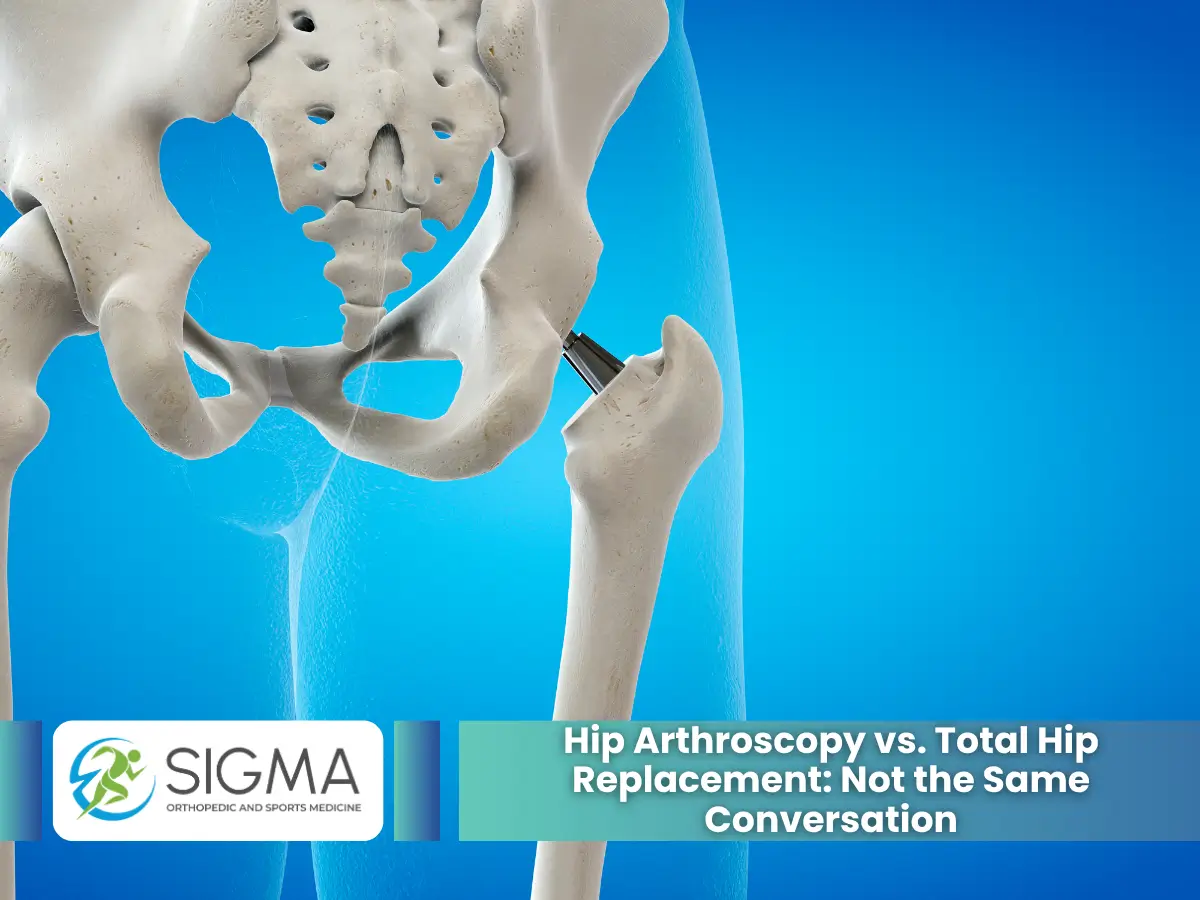
Patients sometimes arrive confused about whether arthroscopy or replacement is being recommended, and it’s an understandable blur. Both involve the hip. Both are surgical. But they address completely different clinical realities.
Total hip replacement is a reconstructive procedure. It removes the damaged joint surfaces and replaces them with prosthetic components. It’s the right answer for end-stage arthritis, significant structural failure, or joint degeneration that has passed the point where preservation is viable. It works well. But it’s irreversible.
Hip arthroscopy is a joint-preserving procedure. The goal is to address the specific pathology, whether a labral tear, impingement, cartilage damage, or loose bodies, while keeping the native joint intact. For patients who are candidates, arthroscopy can delay or,r in some cases, prevent the need for replacement entirely.
The National Institutes of Health (NIH) has published data showing that appropriate patient selection for hip arthroscopy is one of the strongest predictors of outcome. When the right procedure is matched to the right diagnosis at the right stage, results are substantially better than when arthroscopy is applied too late, or replacement is performed prematurely.
Hip Arthroscopy Cost: What the Numbers Don’t Capture
Hip arthroscopy cost varies depending on location, facility, surgeon experience, insurance coverage, and the complexity of the procedure. In the United States, arthroscopic hip procedures typically range from several thousand dollars for straightforward cases to higher figures for complex reconstructions.
Open surgeries and total hip replacements tend to carry higher facility and anesthesia costs, longer inpatient stays, and more extensive post-discharge care needs. When you factor in lost work time, extended rehabilitation, and the downstream costs of complications, the financial comparison often shifts meaningfully.
But here’s the part that cost comparisons miss entirely: the cost of the wrong procedure, or the right procedure done at the wrong stage, doesn’t show up on any initial invoice. It shows up months later in revision surgery, persistent pain, or a joint that never quite recovered the way it should have.
Hip Arthroscopy Rehab Protocol: Why the Recovery Plan Is Part of the Procedure
Surgeons who take arthroscopy seriously don’t hand patients a generic exercise sheet and wish them well. The rehab protocol is clinical, structured, and as individually calibrated as the surgical plan itself.
A well-designed hip arthroscopy rehab protocol typically moves through three phases: tissue protection, progressive loading, and functional restoration. Each phase has specific criteria that must be met before advancing. Rushing a phase because the patient feels fine is one of the most common ways recoveries go sideways.
What that protocol includes matters too. Neuromuscular control exercises, progressive hip strengthening targeting the gluteus medius and deep external rotators, gait retraining, and sport- or activity-specific conditioning aren’t optional add-ons. They’re what turns a technically successful surgery into a functionally successful outcome.
Hip Arthroscopy Success Rate: What the Evidence Actually Shows
Success rates for hip arthroscopy depend heavily on patient selection, surgeon experience, and the specific condition being treated. For labral repair in appropriate candidates, published success rates for significant pain reduction and return to function consistently sit in the 70 to 90 percent range across multiple peer-reviewed studies.
The American Academy of Orthopaedic Surgeons (AAOS) has acknowledged hip arthroscopy as an evidence-supported intervention for specific hip pathologies, with outcomes continuing to improve as surgical technique and patient selection criteria have become more refined over the past decade.
Where outcomes fall short is almost always traceable to one of two things: the procedure was performed on a patient whose condition had already progressed beyond what arthroscopy can address, or the postoperative rehabilitation protocol wasn’t followed with sufficient structure and consistency.
Technique matters. But so does everything that happens after the portal sites close.
Why SIGMA Orthopedics Approaches Hip Surgery Differently

At SIGMA Orthopedics, the conversation about hip arthroscopy doesn’t start with the procedure. It starts with the diagnosis. The SIGMA framework is built on precision evaluation, which means identifying the actual pain generator before any discussion of surgical options takes place.
That matters because a lot of hip surgeries, arthroscopic and open alike, are performed based on imaging findings rather than clinical correlation. An MRI can show a labral tear in a patient whose primary problem is something else entirely. Operating on the finding rather than the cause is a recipe for the kind of outcome nobody wants.
SIGMA’s multi-specialty team, spanning sports medicine, spine, and rehabilitation, collaborates across disciplines before treatment decisions are made. The SIGMA protocol brings together structured diagnosis, evidence-based treatment selection, and milestone-tracked recovery into a coordinated system. Patients don’t just receive a procedure. They receive a plan.
The SynerG Orthobiologics program at SIGMA also means that biologic adjuncts, including options like PRP applied at the time of arthroscopy, are integrated into care pathways where the evidence supports their use, not as upsells, but as components of a comprehensive clinical strategy.
Conclusion
The gap between hip arthroscopy and open surgery isn’t just technical. It’s philosophical. One approach is built around preserving what’s there. The other is built around replacing what’s gone. Both are legitimate. Neither is automatically correct.
What determines the right path is a precise understanding of what’s actually happening inside the joint, at what stage, and in which patient. That kind of clarity doesn’t come from a fifteen-minute consultation or a quick read of an MRI report. It comes from a structured evaluation by a team that’s asked the right questions before picking up any instrument.
If you’re weighing surgical options for hip pain and you’re not certain you’ve received that level of clarity, that uncertainty is worth addressing before you commit to a course of action.
Ready to understand your options with real precision? Request a consultation at SIGMA Orthopedics and get a structured evaluation that starts with an accurate diagnosis, not an assumption. Call 833-SIGMA-MD or book your appointment online.
Frequently Asked Questions
How long does minimally invasive hip surgery recovery time typically take?
Most patients begin weight-bearing with crutches within the first week and progress through rehab over 3 to 6 months. Full recovery depends on the procedure and consistency with rehabilitation.
What is the success rate of minimally invasive hip surgery for labral repair?
Success rates range from 70 to 90 percent for pain relief and improved function in properly selected patients. Outcomes depend on accurate diagnosis and adherence to a structured rehab program.
How does minimally invasive hip surgery cost compared to open surgery?
This type of procedure is usually less expensive due to shorter operating time and no hospital stay. However, proper diagnosis and recovery are key, as revision surgeries can significantly increase costs.
Can minimally invasive hip surgery replace the need for a total hip replacement?
In some cases, yes. It can treat underlying issues and delay or prevent joint replacement when damage is still manageable and addressed early.
What should a minimally invasive hip surgery rehab protocol include?
A proper rehab plan includes phased recovery with protection, strength building, and functional training. It should focus on mobility, muscle control, and gradual return to activity.




